| Journal of Clinical Medicine Research, ISSN 1918-3003 print, 1918-3011 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Clin Med Res and Elmer Press Inc |
| Journal website https://www.jocmr.org |
Case Report
Volume 14, Number 4, April 2022, pages 170-173
Combined Gluteal and Posterior Thigh Compartment Syndrome Without Associated Fracture: A Case Report
Paschalis Gavriilidisa, d, Francisco Reyes Miliana, Damir Kacarevicb, Derek Burkec
aDepartment of Surgery, Saint Helena General Hospital, Jamestown, STHL 1ZZ Saint Helena, South Atlantic Ocean, UK
bDepartment of Anaesthesiology, Saint Helena General Hospital, Jamestown, STHL 1ZZ Saint Helena, South Atlantic Ocean, UK
cDepartment of General Medicine, Saint Helena General Hospital, Jamestown, STHL 1ZZ Saint Helena, South Atlantic Ocean, UK
dCorresponding Author: Paschalis Gavriilidis, Department of Surgery, Saint Helena General Hospital, Jamestown, STHL 1ZZ Saint Helena, South Atlantic Ocean, UK
Manuscript submitted April 13, 2022, accepted April 22, 2022, published online April 30, 2022
Short title: Combined Gluteal and Posterior Thigh Compartment Syndrome
doi: https://doi.org/10.14740/jocmr4725
| Abstract | ▴Top |
Compartment syndrome usually occurs after trauma, fracture, or compression injuries. To the authors’ best knowledge, this is the first reported case in the medical literature of a combined gluteal and posterior thigh compartment syndrome after an accidental fall without an associated fracture. A 65-year-old man attended the emergency department of the general hospital in a remote island complaining of a swollen painful thigh. He reported that 24 h previously he had an accidental slip and fall on his overstretching right leg. Physical examination revealed right posterior thigh edema, tenderness, paraesthesia, and firmness to palpation. Any attempt to flex the knee provoked pain of intensity 10/10. In addition, there was blue discoloration over the lower half of the gluteal region, non-compressible tense swelling, and pain of intensity 10/10 elicited with passive range of motion of the hip. Compartment syndrome was considered and consequently, fasciotomy of the gluteal and posterior thigh compartments was performed under spinal anesthesia. Compartment syndrome is a surgical emergency. In a remote island, it must be considered and treated early because any delayed diagnosis may lead to loss of an extremity, kidney failure, sepsis and even death.
Keywords: Posterior thigh compartment; Gluteal compartment; Compartment syndrome; Fasciotomy
| Introduction | ▴Top |
Gluteal compartment syndrome usually occurs after vascular injury, surgical positioning, and prolonged immobilization from alcohol or drug immobilization [1-3]. Early diagnosis and treatment may prevent sciatic nerve palsy and life-threatening hyperkalemia secondary to rhabdomyolysis [4, 5].
Thigh compartment syndrome is relatively rare. So far only 80 cases have been reported in the literature [6]. Due to the large volume of the thigh compartments and the fact that they blend with the compartments of the hip and gluteal regions, a large volume of blood is needed to produce a compartment syndrome [6, 7].
The commonest causes of compartment syndrome of the thigh without associated femoral fracture are anticoagulant medications, hemophilia, human immunodeficiency virus (HIV) infection and hepatitis [8].
This paper presents the first case in the international literature of combined gluteal and posterior thigh compartment syndrome secondary to blunt trauma after accidental fall on overstretching leg without an associated fracture.
| Case Report | ▴Top |
A 65-year-old man presented to emergency department of the general hospital in a remote island with painful swollen right posterior thigh, with heart rate of 94, respiratory rate of 18, blood pressure of 100/69 mm Hg, hemoglobin (Hb) of 10.6 g/dL, and hematocrit (Ht) of 32%. His past medical history included type II diabetes mellitus, chronic obstructive pulmonary disease (COPD), obstructive sleep apnea, chronic respiratory acidosis, myocardial infarction, and coronary stenting in 2019. He reported that 24 h previously he fell accidentally on his overstretched right leg. Over first day post-injury, he did not have any functional disability of the leg. However, the next day he was not able to walk because his thigh became swollen from the gluteal fold to the end of the popliteal fossa. Inspection of the leg revealed blue discoloration over the gluteal fold, the lower third of the posterior thigh, and the popliteal fossa (Fig. 1). In addition, physical examination revealed edema, pain, paraesthesia, and firmness on palpation. Hip motion and knee flexion provoked pain of intensity 10/10. Femoral and dorsalis pedis arteries were palpable and normal, and the popliteal artery was not palpable due to edema in the popliteal fossa. His laboratory results showed international normalized ratio (INR) of 1.18 (0.9 - 1.2), activated partial thromboplastin time (aPTT) of 25.3 s (22 - 31), prothrombin time of 11.4 s (9 - 12), white blood cells (WBCs) of 6.9, neutrophils of 5.9, glomerular filtration rate (GFR) of 140.79 mL/min, Na of 138 mmol/L, K of 4.2 mmol/L, Cr of 60 µmol/L, low-density lipoprotein (LDL) of 1.09 mmol/L, high-density lipoprotein (HDL) of 3.71 mmol/L, and hemoglobin A1c (HbA1c) of 52 (20 - 42) mmol/mol. Patient is not a smoker, his body mass index (BMI) is 38 and he was on the following medications: aspirin dispersible 75 mg, atorvastatin 80 mg, bisoprolol fumarate 5 mg, lisinopril 20 mg, metformin hydrochloride 500 mg, and doxazosin mesylate 2 mg. Compartment syndrome was considered. The patient underwent fasciotomy of the gluteal and posterior thigh compartments under spinal anesthesia. The operation was uneventful, and he was transferred to the high dependency unit. The limb was elevated on five pillows to reduce the edema sustained from the compartment syndrome with the aim to review within the first 4 days for possible primary closure. Because of the COPD, obstructive sleep apnea and chronic respiratory acidosis, the patient needed 24-h supplemental oxygen. His vital signs remained stable. On the fourth postoperative day, the surgical wound was assessed, and it was found that the muscles were edematous. Skin pinching was performed and the skin laxity around the wound was found to be unsatisfactory with persistent edema of the muscles of the right posterior thigh. We decided to abandon any attempt at primary closure and referred the patient to a tertiary referral center for multimodality treatment care.
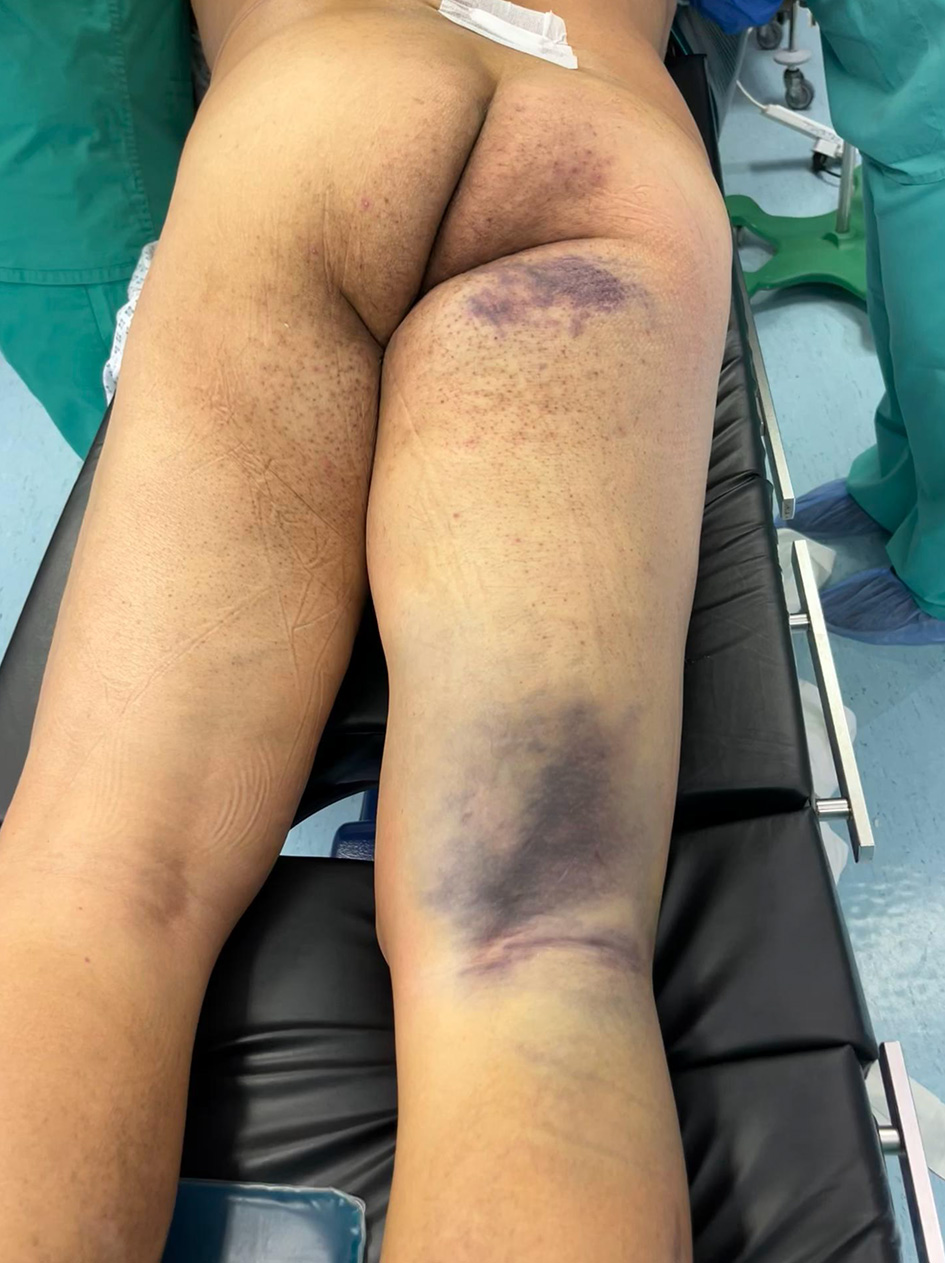 Click for large image | Figure 1. Bruising over the right gluteal, upper, and lower posterior thigh. Remarkable edema is noted. Physical examination revealed pain, paraesthesia, and firmness on the palpation. Hip motion and knee flexion elicited pain 10/10. |
| Discussion | ▴Top |
Compartment syndrome is surgical emergency requiring early diagnosis and intervention. The diagnosis is mainly based on detailed history, physical examination, and consequently sound clinical judgement. It has been reported that fractures (69%) and soft tissue injuries (23%) are the most common causes of the compartment syndrome [9]. Gluteal compartment syndrome most commonly occurs secondary to drug/alcohol intoxication or surgical positioning, and traumatic injury represents only 20% of cases [1-3].
The 5 - 6 diagnostic Ps (pain, pressure, pulselessness, paralysis, paraesthesia, and pallor) are described as the characteristic signs and symptoms of the compartment syndrome [10, 11]. However, they may be absent in 50% of the cases [10]. Notably, an analysis of four prospective studies including 132 patients with compartment syndrome reported that the positive predictive value of the pain, paraesthesia, and paresis was only 11-15%, whereas the negative predictive value was 98% [12]. Any use of local anesthetics may mask alarming neurologic symptoms and pain secondary from increasing compartment pressures [13]. It has been reported that epidural analgesia may increase the risk of developing compartment syndrome [14, 15]. Differential pressure between compartments and perfusion pressure less than 30 mm Hg is a reliable indication for fasciotomy [16]. Heckman et al reported that pressure measurements a few centimeters from a fracture site may produce unreliable results [17].
Considering all the above information, we can conclude that diagnosis of compartment syndrome in most cases is a diagnostic dilemma and a troubling situation for any surgeon. The presence of signs of pain and pressure on the extremity should be high suspicious not only in cases of high-energy traumas and crush-injuries but also for unusual conditions and circumstances.
In our patient, we considered the diagnosis of compartment syndrome based only on detailed history, the signs and symptoms elicited in the physical examination and clinical judgement. At the time the patient presented, there was no radiologist in the hospital. We were therefore without the benefit of any imaging evidence or needle intra-compartmental monitoring, and the diagnosis was based purely on clinical judgement.
O’Toole et al demonstrated that the diagnostic rate of compartment syndrome of tibial fractures in a level I trauma center ranged between 2% and 24% [11].
Any misjudgement and delayed intervention may result in the loss of an extremity, renal failure, sepsis, and death [18, 19]. The commonest complications that may lead to high medical costs and medicolegal indemnity cases are infections, muscle necrosis/contractures, fracture non-union, nerve injury, chronic pain, and amputation [20, 21].
In addition to the difficulty with making the diagnosis of the compartment syndrome is the decision whether to close the fasciotomy wound.
There are no predictive algorithms and clinical guidelines for the best approach for wound closure. A number of techniques have been used for wound closure. The most common approach is the split-thickness skin grafting [22]. Vacuum-assisted closure (VAC) is also widely used but it has been reported that VAC fails to provide adequate skin approximation for final closure; therefore, the patient often needs to undergo an additional intervention [23].
Six innovative techniques based on dermal apposition are listed, namely Ty-Rap (Thomas & Betts, USA) [23], vessel loop shoelace technique [24], subcuticular suture [25], dynamic wound closure (Canica design Inc., Canada) [26], Sure-closure (Life Medical Sciences Inc., USA) [27], STAR (WoundTEK Inc., USA) [27], and silver bullet wound closure device (Boehringer Laboratories, USA) [28]. Bengezi and Vo proposed elevation to alleviate the edema, skin pinching to assess whether the laxity of the skin is satisfactory and consequently wound closure [29].
In our case, after detailed assessment of all the above techniques, we decided to assess the elevation technique because it is less invasive and there is no need for additional materials. The assessment of the wound on fourth postoperative day revealed that it did not fulfil the criteria for safe primary closure. Therefore, for the best interest of the patient, we decided to transfer him in referral center for multimodality treatment care.
Up to authors’ best knowledge, this is the first case in the literature that describes a combined gluteal and posterior thigh compartment syndrome not associated to fracture provoked by blunt trauma. Of note, patient’s clotting profile at presentation was normal.
Conclusions
Diagnosis and management of compartment syndrome is a troubling situation for any involved clinician. In a remote island, early diagnosis will prevent major complications and save the life of patient. Predictive algorithms and sound clinical guidelines are urgently needed.
Learning points
Signs of pressure and pain in any trauma patients should raise suspicion for compartment syndrome.
Close monitoring and clinical judgement by the same doctor every 2 - 4 h are the best tools to manage suspected compartment syndrome.
Worsening pain aggravated by passive muscle stretch is a cardinal sign for diagnosis.
Continuous pressure monitoring is recommended for all patients at risk for developing acute compartment syndrome.
Fasciotomy is the treatment of choice and must be performed in standardized way to protect key functional structures.
Acknowledgments
None to declare.
Financial Disclosure
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflict of Interest
None to declare.
Informed Consent
Patient consented his case to be published anonymized in the medical literature.
Author Contributions
PG contributed to conceptualization, formal analysis, investigation, methodology, software, validation, writing-original draft, editing, and approval; FRM and DK contributed to formal analysis, investigation, validation, editing, and approval; DB contributed to conceptualization, formal analysis, investigation, methodology, software, validation, writing-original draft, editing, approval, and supervision.
Data Availability
The authors declare that data supporting the findings of this study are available within the article.
| References | ▴Top |
- Hynes JE, Jackson A. Atraumatic gluteal compartment syndrome. Postgrad Med J. 1994;70(821):210-212.
doi pubmed - Iizuka S, Miura N, Fukushima T, Seki T, Sugimoto K, Inokuchi S. Gluteal compartment syndrome due to prolonged immobilization after alcohol intoxication: a case report. Tokai J Exp Clin Med. 2011;36(2):25-28.
- Diaz Dilernia F, Zaidenberg EE, Gamsie S, Taype Zamboni DE, Carabelli GS, Barla JD, Sancineto CF. Gluteal compartment syndrome secondary to pelvic trauma. Case Rep Orthop. 2016;2016:2780295.
doi pubmed - Lawrence JE, Cundall-Curry DJ, Stohr KK. Delayed presentation of gluteal compartment syndrome: the argument for fasciotomy. Case Rep Orthop. 2016;2016:9127070.
doi pubmed - Targa L, Droghetti L, Caggese G, Zatelli R, Roccella P. Rhabdomyolysis and operating position. Anaesthesia. 1991;46(2):141-143.
doi pubmed - Suzuki T, Moirmura N, Kawai K, Sugiyama M. Arterial injury associated with acute compartment syndrome of the thigh following blunt trauma. Injury. 2005;36(1):151-159.
doi pubmed - Schwartz JT, Jr., Brumback RJ, Lakatos R, Poka A, Bathon GH, Burgess AR. Acute compartment syndrome of the thigh. A spectrum of injury. J Bone Joint Surg Am. 1989;71(3):392-400.
doi pubmed - Hope MJ, McQueen MM. Acute compartment syndrome in the absence of fracture. J Orthop Trauma. 2004;18(4):220-224.
doi pubmed - McQueen MM, Gaston P, Court-Brown CM. Acute compartment syndrome. Who is at risk? J Bone Joint Surg Br. 2000;82(2):200-203.
doi pubmed - Seddon HJ. Volkmann's ischaemia in the lower limb. J Bone Joint Surg Br. 1966;48(4):627-636.
doi pubmed - O'Toole RV, Whitney A, Merchant N, Hui E, Higgins J, Kim TT, Sagebien C. Variation in diagnosis of compartment syndrome by surgeons treating tibial shaft fractures. J Trauma. 2009;67(4):735-741.
doi pubmed - Ulmer T. The clinical diagnosis of compartment syndrome of the lower leg: are clinical findings predictive of the disorder? J Orthop Trauma. 2002;16(8):572-577.
doi pubmed - Eyres KS, Hill G, Magides A. Compartment syndrome in tibial shaft fracture missed because of a local nerve block. J Bone Joint Surg Br. 1996;78(6):996-997.
doi pubmed - Mubarak SJ, Wilton NC. Compartment syndromes and epidural analgesia. J Pediatr Orthop. 1997;17(3):282-284.
doi - Price C, Ribeiro J, Kinnebrew T. Compartment syndromes associated with postoperative epidural analgesia. A case report. J Bone Joint Surg Am. 1996;78(4):597-599.
doi pubmed - Maher M, Mauffrey C. Diagnostic dilemma for the orthopedic surgeon. In: Mauffrey C, Hak DJ, Martin IM, eds. Compartment syndrome: a guide to diagnosis and management. Cham (CH). 2019; p. 1-7.
doi - Heckman MM, Whitesides TE, Jr., Grewe SR, Rooks MD. Compartment pressure in association with closed tibial fractures. The relationship between tissue pressure, compartment, and the distance from the site of the fracture. J Bone Joint Surg Am. 1994;76(9):1285-1292.
doi pubmed - Garner MR, Taylor SA, Gausden E, Lyden JP. Compartment syndrome: diagnosis, management, and unique concerns in the twenty-first century. HSS J. 2014;10(2):143-152.
doi pubmed - Taylor RM, Sullivan MP, Mehta S. Acute compartment syndrome: obtaining diagnosis, providing treatment, and minimizing medicolegal risk. Curr Rev Musculoskelet Med. 2012;5(3):206-213.
doi pubmed - Schmidt AH. The impact of compartment syndrome on hospital length of stay and charges among adult patients admitted with a fracture of the tibia. J Orthop Trauma. 2011;25(6):355-357.
doi pubmed - Bhattacharyya T, Vrahas MS. The medical-legal aspects of compartment syndrome. J Bone Joint Surg Am. 2004;86(4):864-868.
doi pubmed - Zannis J, Angobaldo J, Marks M, DeFranzo A, David L, Molnar J, Argenta L. Comparison of fasciotomy wound closures using traditional dressing changes and the vacuum-assisted closure device. Ann Plast Surg. 2009;62(4):407-409.
doi pubmed - Govaert GA, van Helden S. Ty-raps in trauma: a novel closing technique of extremity fasciotomy wounds. J Trauma. 2010;69(4):972-975.
doi pubmed - Zorrilla P, Marin A, Gomez LA, Salido JA. Shoelace technique for gradual closure of fasciotomy wounds. J Trauma. 2005;59(6):1515-1517.
doi pubmed - Chiverton N, Redden JF. A new technique for delayed primary closure of fasciotomy wounds. Injury. 2000;31(1):21-24.
doi - Taylor RC, Reitsma BJ, Sarazin S, Bell MG. Early results using a dynamic method for delayed primary closure of fasciotomy wounds. J Am Coll Surg. 2003;197(5):872-878.
doi - McKenney MG, Nir I, Fee T, Martin L, Lentz K. A simple device for closure of fasciotomy wounds. Am J Surg. 1996;172(3):275-277.
doi - Medina C, Spears J, Mitra A. The use of an innovative device for wound closure after upper extremity fasciotomy. Hand (N Y). 2008;3(2):146-151.
doi pubmed - Bengezi O, Vo A. Elevation as a treatment for fasciotomy wound closure. Can J Plast Surg. 2013;21(3):192-194.
doi pubmed
This article is distributed under the terms of the Creative Commons Attribution Non-Commercial 4.0 International License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Clinical Medicine Research is published by Elmer Press Inc.


