| Journal of Clinical Medicine Research, ISSN 1918-3003 print, 1918-3011 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Clin Med Res and Elmer Press Inc |
| Journal website http://www.jocmr.org |
Case Report
Volume 8, Number 2, February 2016, pages 168-174
Clostridium septicum Aortitis of the Infrarenal Abdominal Aorta
Aditya Shaha, b, Tariq Yousufa, Mohammed Rachida, Naureen Alia, Muhammad Tabriza, Kevin Loughrya
aAdvocate Christ Medical Center, 4440 W. 95th Street, Oak Lawn, IL 60453, USA
bCorresponding Author: Aditya Shah, Advocate Christ Medical Center, 4440 W. 95th Street, Oak Lawn, IL 60453, USA
Manuscript accepted for publication December 18, 2015
Short title: Clostridium septicum Aortitis
doi: http://dx.doi.org/10.14740/jocmr2435w
| Abstract | ▴Top |
Clostridium septicum aortitis is a rare infection that has a strong association with occult colonic malignancy. There is also emerging evidence to support the combination of medical and surgical management over medical management alone. To the best of our knowledge, we report the 40th known case of C. septicum aortitis.
Keywords: Aortitis; Colonic malignancy; Clostridium septicum
| Introduction | ▴Top |
Clostridium septicum (C. septicum) can cause a wide array of clinical manifestations including gas gangrene. One proposed mechanism of infection is by hematogenous spread from the gastrointestinal tract. Gas gangrene caused by C. septicum is associated with colorectal cancer and other defects of the bowel. Alpern et al and Kornbluth et al have reported an association between C. septicum infection and malignancy [1, 2]. We describe a rare case of C. septicum-induced aortitis affecting the infrarenal abdominal aorta. We received consent from the patient for publication of this case.
C. septicum is a Gram-positive, spore forming, obligate, anaerobic bacterium. C. septicum causes myonecrosis through the release of exotoxins such as the alpha toxin [3], lethal toxin, and hemolytic toxin.
An infected aneurysm, also known as a “mycotic aneurysm” or “microbial arteritis”, is an aneurysm arising from bacterial infection of the arterial wall. It was described first by Osler in 1887 [4]. This complication is not all that uncommon and it is caused by the hematogenous spread of bacterial infection. Given that the current treatment modalities for aortic aneurysms may be time sensitive, early diagnosis is prudent. Without medical or surgical management, severe hemorrhage, rupture, or uncontrolled sepsis may occur [5]. Despite this, symptomatology is frequently nonspecific during the early stages so a high index of suspicion is required to make the diagnosis.
We present a case of a 78-year-old patient who was found to have an incidental aortitis in the setting of intussusception and colon cancer.
| Case Report | ▴Top |
The patient was a 78-year-old male who presented with chronic diarrhea of 2 years’ duration. He initially presented to his gastroenterologist who performed a colonoscopy and discovered colonic cancer at the hepatic flexure. Pathology revealed moderately differentiated adenocarcinoma with complex focally cribriform glands formed by cells with enlarged hyperchromatic nuclei. The patient was then admitted to the hospital for further workup and staging of the malignancy.
On admission, the patient had a fever of 39.0 °C, heart rate of 96 beats/min, hemoglobin of 12 mg/dL, and leukocytosis of 17,000/μL. Tumor marker carcinoembryonic antigen was 137 μg/L.
He underwent a CT scan for further malignancy staging and was found to have an intussusception at the location of his newly discovered colonic cancer (Fig. 1).
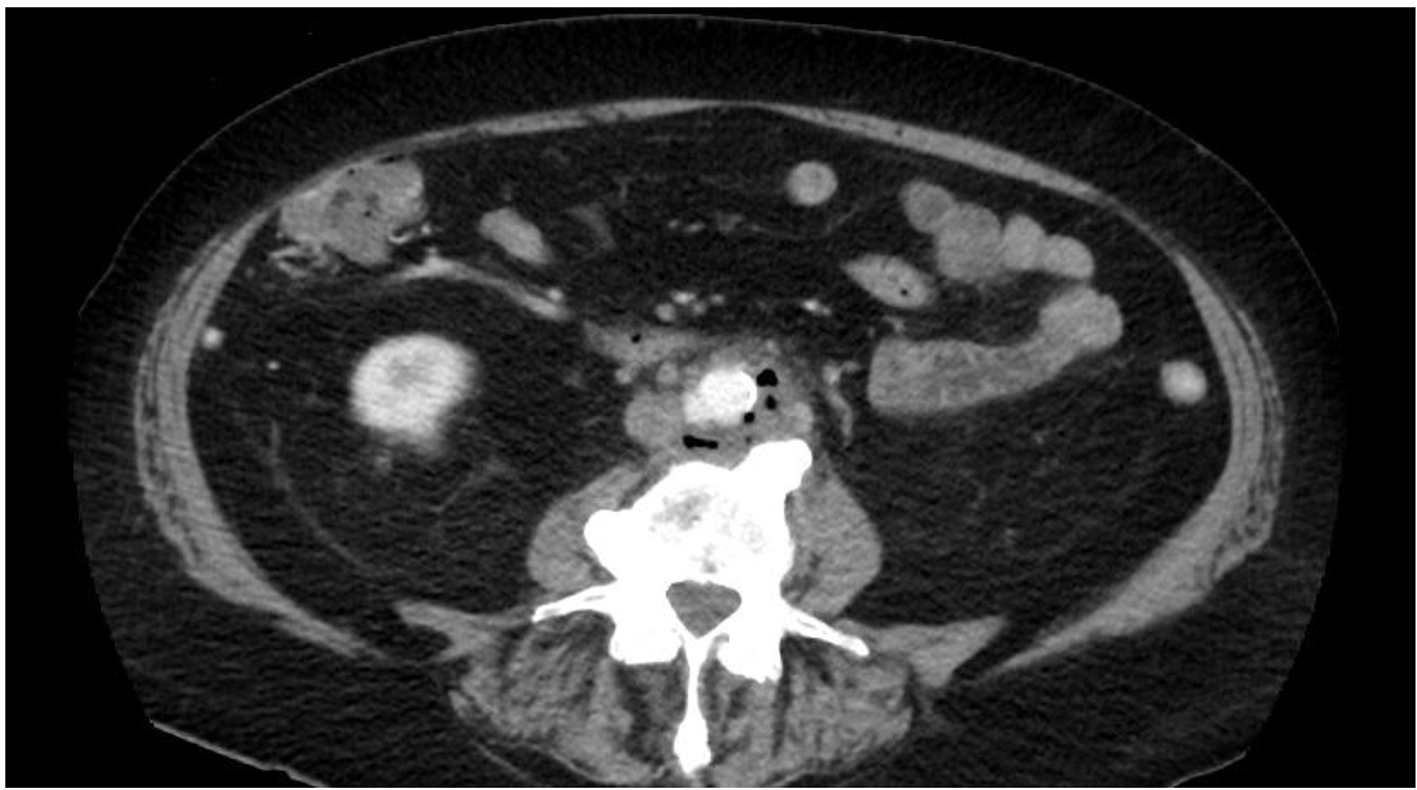 Click for large image | Figure 1. Coronal CT showing intussusception at the junction between the transverse colon and the hepatic flexure. |
The CT scan also incidentally revealed findings consistent with aortitis with a periaortic abscess and an asymptomatic pseudoaneurysm in the infrarenal abdominal aorta (Fig. 2 and 3). Blood cultures also grew C. septicum which was pan-susceptible. On further questioning, the patient endorsed a 10 pound weight loss over the preceding few months with intermittent explosive diarrhea along with decreased appetite, weakness, and generalized malaise. The patient denied other constitutional symptoms such as fever or chills. Prompt resection of the infrarenal aorta was performed. Pre- and post-operatively the patient was started on intravenous aztreonam, vancomycin, and metronidazole and sent home on oral metronidazole. In the interim, he also underwent elective definitive management of his neoplasia with colon resection of the hepatic flexure mass.
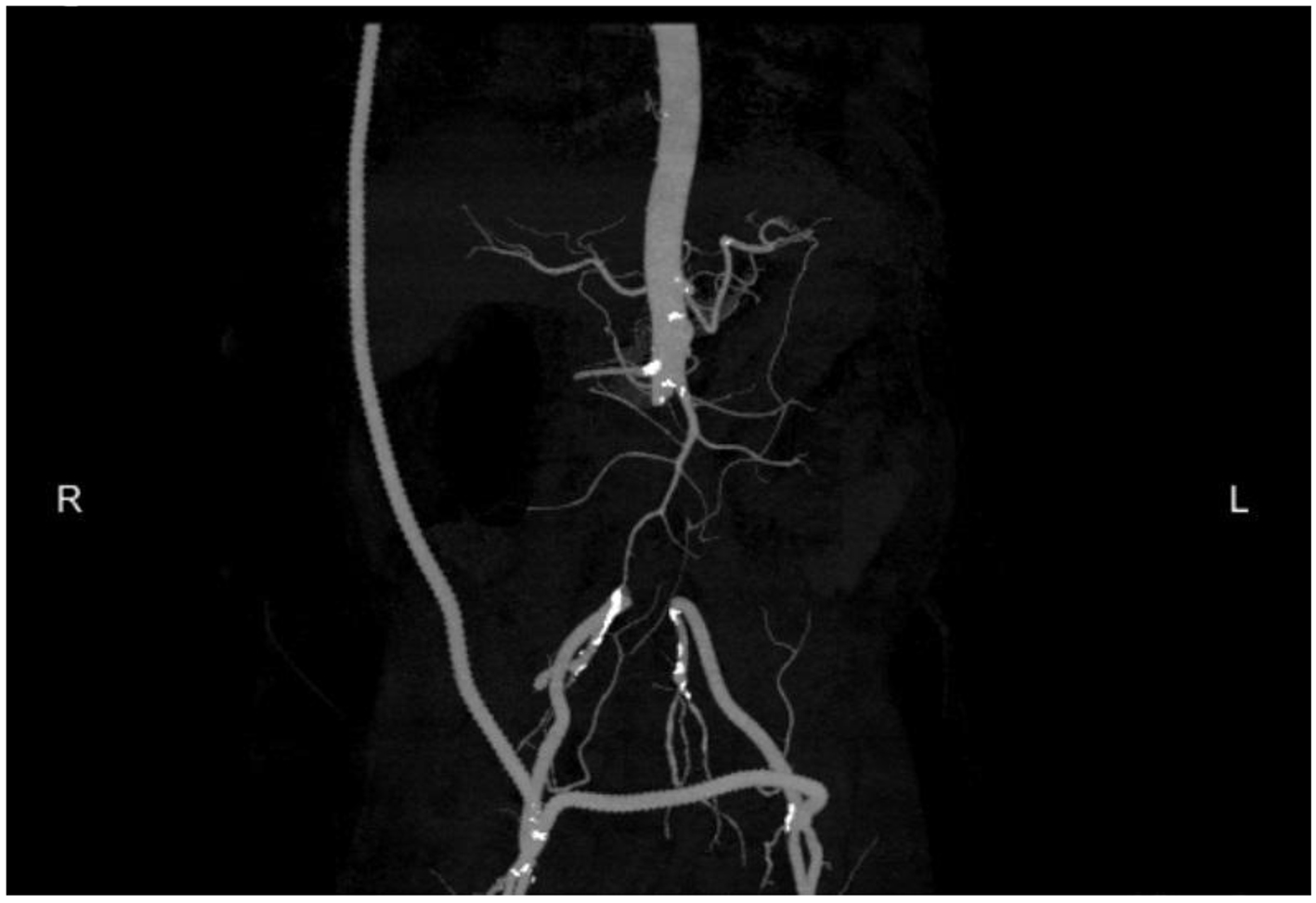 Click for large image | Figure 2. Aortitis with periaortic abscess and a pseudo aneurysm in the infrarenal abdominal aorta. |
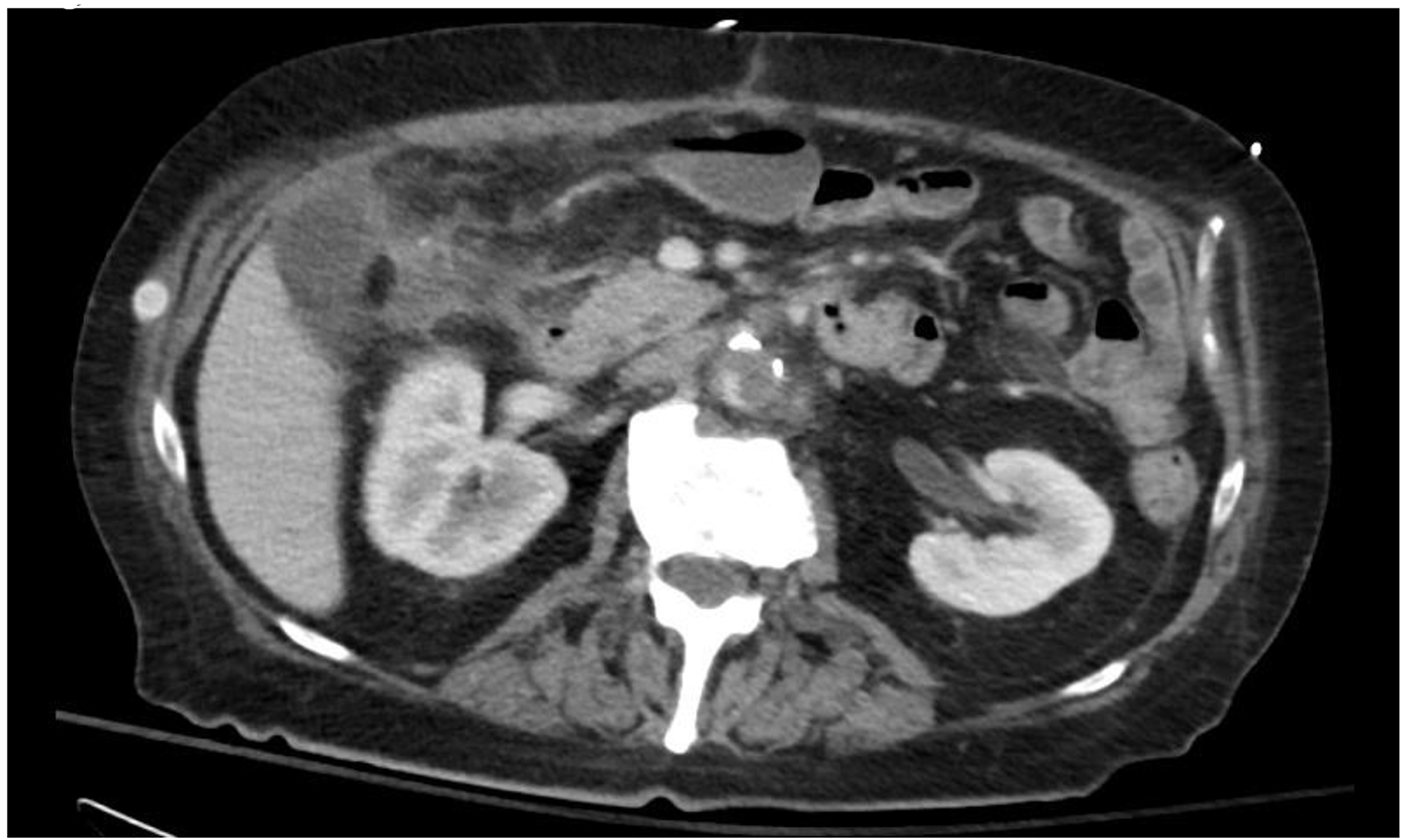 Click for large image | Figure 3. Coronal CT showing mycotic aneurysm of the infrarenal aorta with gas bubbles. |
The patient was doing well post-operatively for several months undergoing meticulous multi-disciplinary care until he started developing fevers, chills, and weakness. He presented back to the hospital and was found to have an abscess at the post-operative anastomotic site of the colon cancer resection at the hepatic flexure. Blood cultures were drawn which regrew C. septicum. He was managed with the same combination of intravenous antibiotics and was discharged home on oral metronidazole and levofloxacin. The plan was to continue the current antibiotics and to do a follow-up CT scan to confirm the response of the abscess to the proposed treatment.
| Discussion | ▴Top |
A typical finding of clostridial mycotic aneurysms in the CT scan is gas formation surrounding the aorta or peripheral arteries. Clostridia can proliferate in tissues when oxidation-reduction falls or the pH is reduced, which may occur with arterial injury, necrotic tissue, or anoxic tissue with lactic acid accumulation [6]. For this reason, clostridial infection is frequently associated with gastrointestinal or hematologic malignancy. Kornbluth et al reported an associated malignancy in 81% of patients with C. septicum infection, which has been validated by other similar studies [2]. A study of human fecal flora in healthy volunteers showed that C. septicum is not normally present [7]. Only about 1.3% of clostridial infections are caused by C. septicum [8]. It is believed that ulcerative lesions of the gastrointestinal tract, especially colon carcinoma, can allow clostridial organisms to enter the bloodstream and seed an atherosclerotic focus in the aorta, resulting in the development of mycotic aortic aneurysm [9]. Therefore, the diagnosis of clostridial mycotic aortic aneurysm requires a thorough search for an occult malignancy.
Of the total 40 cases of aortitis caused by C. septicum that have been reported and listed in Table 1 [9-46], at the time of the review the aneurysm was located in the infrarenal aorta in 13 (34.2%), abdominal aorta (including juxtarenal and suprarenal) in nine (23.6%), the thoracic aorta (ascending part and the aortic arch) in 10 (26.3%), the iliac artery in three, the thoracoabdominal in two, the whole aorta in two, the popliteal artery in one, and the thoracic aorta and abdominal aorta (double aneurysm) in one patient. Of these 40 cases, seven cases experienced aortic dissection and one case experienced aortic rupture. Also, two cases were reported in young age (16 years old and 22 years old) and both of them ended up in aortic dissection and death. In these 40 cases, there were 30 cases (78.9%) with colon neoplasm. Twenty-two of the 24 patients who underwent vascular surgery survived (91.6% survival rate, 8.4% mortality rate), whereas four out of five cases that treated medically only died (80% mortality). Out of these 40 cases, 10 cases died before getting accurate diagnosis, diagnosed at autopsy, or did not make it till the time of the surgical intervention. Surgical treatment seems to be needed to achieve optimal results.
 Click to view | Table 1. Cases of Aortitis Caused by C. septicum |
The traditional surgical dictum mandates excision of the infected aneurysm, wide local debridement, administration of antibiotics, and remote grafting in the form of extra-anatomic bypass through a clean surgical field. However, in situ reconstruction has received emphasis in recent years. In the presence of a positive gram stain or purulence, excision of the pseudo aneurysm with an extra-anatomic bypass should be used, followed by a 6-week course, at the minimum, of parenteral antibiotics. In the absence of purulence and with a negative gram stain, in situ graft reconstruction with synthetic material can be utilized, followed by a 6- to 8-week course of organism-specific antibiotics [20].
Our patient had an emergent right axillofemoral bypass with an 8 mm heparin bonded polytetrafluoroethylene (PTFE). Abdominal aortic exploration and ligation of the infrarenal abdominal aorta was performed with aortic debridement. Thrombectomy of the right axillofemoral bypass was also performed and the peripheral perfusion was left intact. As per current treatment guidelines, the patient then received long-term parenteral antibiotics with aztreonam, vancomycin and metronidazole [9]. He was eventually transitioned to only oral metronidazole and continued to clinically improve up until the discontinuation of antibiotics.
Conclusion
Our literature review revealed that surgical and medical management (8.4% mortality rate) was superior to medical management alone (80% mortality rate) in patients with this rare condition which is summarized in Table 2. Consideration of immediate surgical management in addition to medical management of these patients should be given.
 Click to view | Table 2. Summary of Surgical and Medical Management |
Owing to the rare nature of the condition, and most cases being managed with a combination of medical and surgical management, one limitation of our conclusion could be that the number of patients treated only medically might be too small to make a confirmed recommendation of the treatment goals and standards going forward.
In conclusion, our case is one of few reported cases of aortic aneurysm related to clostridium bacteremia. Most of the reported cases in the literature have been associated with colonic malignancy like in our patient. Hence, it would be prudent for clinicians to do a thorough search for malignant processes in patients presenting with similar complaints and C. septicum bacteremia, and also give serious consideration to prompt surgical management of the same.
Disclaimer
The authors have no financial or proprietary interest in the subject matter of this article.
Source of Funding
None.
| References | ▴Top |
- Alpern RJ, Dowell VR, Jr. Clostridium septicum infections and malignancy. JAMA. 1969;209(3):385-388.
doi pubmed - Kornbluth AA, Danzig JB, Bernstein LH. Clostridium septicum infection and associated malignancy. Report of 2 cases and review of the literature. Medicine (Baltimore). 1989;68(1):30-37.
doi - Kennedy CL, Krejany EO, Young LF, O'Connor JR, Awad MM, Boyd RL, Emmins JJ, et al. The alpha-toxin of Clostridium septicum is essential for virulence. Mol Microbiol. 2005;57(5):1357-1366.
doi pubmed - Osler W. The Gulstonian Lectures, on Malignant Endocarditis. Br Med J. 1885;1(1262):467-470.
doi pubmed - Muller BT, Wegener OR, Grabitz K, Pillny M, Thomas L, Sandmann W. Mycotic aneurysms of the thoracic and abdominal aorta and iliac arteries: experience with anatomic and extra-anatomic repair in 33 cases. J Vasc Surg. 2001;33(1):106-113.
doi pubmed - Schaaf RE, Jacobs N, Kelvin FM, Gallis HA, Akwari O, Thompson WM. Clostridium septicum infection associated with colonic carcinoma and hematologic abnormality. Radiology. 1980;137(3):625-627.
doi pubmed - Moore WE, Holdeman LV. Human fecal flora: the normal flora of 20 Japanese-Hawaiians. Appl Microbiol. 1974;27(5):961-979.
pubmed - Bodey GP, Rodriguez S, Fainstein V, Elting LS. Clostridial bacteremia in cancer patients. A 12-year experience. Cancer. 1991;67(7):1928-1942.
doi - Seder CW, Kramer M, Long G, Uzieblo MR, Shanley CJ, Bove P. Clostridium septicum aortitis: Report of two cases and review of the literature. J Vasc Surg. 2009;49(5):1304-1309.
doi pubmed - Bridges RA, McTamaney JP, Barnes RW. Recognition and management of ruptured infected aneurysm of the abdominal aorta. Vasc Surg. 1981;15:360-366.
doi - Semel L, Aikman WO, Parker FB, Jr., Marvasti MA. Nontraumatic clostridial myonecrosis and mycotic aneurysm formation. N Y State J Med. 1984;84(4):195-196.
pubmed - Kaufman JL, Fereshetian A, Chang B, Shah DM, Leather RP. Septicemia presenting with endoaneurysmal gas: CT demonstration. AJR Am J Roentgenol. 1988;151(2):287-288.
doi pubmed - Narula A, Lake SP, Baker AR, Greenwood RK. Mycotic aneurysm of the popliteal artery following right hemicolectomy. Postgrad Med J. 1988;64(754):638-639.
doi pubmed - Momont SL, Overholt EL. Aortitis due to metastatic gas gangrene. Wis Med J. 1989;88(12):28-30.
pubmed - Asplund MW, Molinaro A. Infected solitary iliac artery aneurysm. J Vasc Surg. 1990;12(2):219-220.
doi - Skipper D, Birch HA, Fallowfield ME, Taylor RS. Clostridial mycotic aneurysm of the suprarenal abdominal aorta. J Cardiovasc Surg (Torino). 1991;32(4):472-474.
- Brahan RB, Kahler RC. Clostridium septicum as a cause of pericarditis and mycotic aneurysm. J Clin Microbiol. 1990;28(10):2377-2378.
pubmed - Hurley L, Howe K. Mycotic aortic aneurysm infected by Clostridium septicum--a case history. Angiology. 1991;42(7):585-589.
doi pubmed - Christensen J, Bistrup C. Case report: emphysematous pyelonephritis caused by clostridium septicum and complicated by a mycotic aneurysm. Br J Radiol. 1993;66(789):842-843.
doi pubmed - Messa CA, 3rd, Kulkarni M, Arous E. Double clostridial mycotic aneurysms of the aorta. Cardiovasc Surg. 1995;3(6):687-692.
doi - Murphy DP, Glazier DB, Krause TJ. Mycotic aneurysm of the thoracic aorta caused by Clostridium septicum. Ann Thorac Surg. 1996;62(6):1835-1837.
doi - Sailors DM, Eidt JF, Gagne PJ, Barnes RW, Barone GW, McFarland DR. Primary Clostridium septicum aortitis: a rare cause of necrotizing suprarenal aortic infection. A case report and review of the literature. J Vasc Surg. 1996;23(4):714-718.
doi - Monsen T, Palmgren H, Arnerlov C, Billheden J. Aortic dissection due to Clostridium septicum infection. Eur J Vasc Endovasc Surg. 1997;13(5):517-518.
doi - Montoya FJ, Weinstein-Moreno LF, Johnson CC. Mycotic thoracic aneurysm due to Clostridium septicum and occult adenocarcinoma of the cecum. Clin Infect Dis. 1997;24(5):785, 1007.
- Cohen CA, Almeder LM, Israni A, Maslow JN. Clostridium septicum endocarditis complicated by aortic-ring abscess and aortitis. Clin Infect Dis. 1998;26(2):495-496.
doi pubmed - Johnson FE. Infected aortic aneurysm. Am J Surg. 1999;178(4):268.
doi - Morrison RC, Jr., DiMuzio PJ, Kahn M, Carabasi RA, 3rd, Bailey W, Edie RN. Clostridial mycotic aneurysm of the thoracoabdominal aorta--a case report. Vasc Surg. 2001;35(4):303-310.
doi pubmed - Al Bahrani BJ, Thomas DJ, Moylan EJ. What's causing that gas? Med J Aust. 2001;174(12):652.
pubmed - Zenati MA, Bonanomi G, Kostov D, Lee R. Images in cardiovascular medicine. Fulminant Clostridium septicum aortitis. Circulation. 2002;105(15):1871.
doi pubmed - Munshi IA, Rhee SW, Pane T, Granowitz E. Clostridium septicum mycotic aortic aneurysm. Am J Surg. 2002;184(1):54-55.
doi - Takano H, Taniguchi K, Kuki S, Nakamura T, Miyagawa S, Masai T. Mycotic aneurysm of the infrarenal abdominal aorta infected by Clostridium septicum: a case report of surgical management and review of the literature. J Vasc Surg. 2003;38(4):847-851.
doi - Liechti ME, Schob O, Kacl GM, Caduff B. Clostridium septicum aortitis in a patient with colon carcinoma. Eur J Clin Microbiol Infect Dis. 2003;22(10):632-634.
doi pubmed - Davies M, Byrne J, Harvey JS. Clostridial infection of the abdominal aorta. J Am Coll Surg. 2003;197(2):331.
doi - Rucker CM, Menias CO, Bhalla S, Geraghty P, Heiken JP. Clostridium septicum infrarenal aortitis secondary to occult cecal adenocarcinoma. AJR Am J Roentgenol. 2004;183(5):1316-1318.
doi pubmed - Evans LT, Chey WD. Clostridial aortitis and colon cancer. Gastrointest Endosc. 2004;60(5):803.
doi - Creed M. Rucker, Christine O. Menias, Sanjeev Bhalla, Patrick Geraghty, Jay P. Heiken. Clostridium septicum. Infrarenal Aortitis Secondary to Occult Cecal Adenocarcinoma.
- Mohamed HK, Elliott BM, Brothers TE, Robison JG. Suprarenal Clostridium septicum aortitis with rupture and simultaneous colon cancer. Ann Vasc Surg. 2006;20(6):825-829.
doi pubmed - Asciutto G, Geier B, Marpe B, Hummel T, Mumme A. A case of contained ruptured aortitis due to Clostridium septicum infection in a patient with a colon malignancy. Chir Ital. 2007;59(5):743-746.
pubmed - Yang Z, Reilly SD. Clostridium septicum aortitis causing aortic dissection in a 22-year-old man. Tex Heart Inst J. 2009;36(4):334-336.
pubmed - Eplinius F, Hadrich C. Acute aortic dissection caused by Clostridium septicum aortitis. Forensic Sci Int. 2014;244:e38-41.
doi pubmed - Moseley B, Mwirigi NW, Bowen J. Clostridium septicum Aortitis and Cecal Adenocarcinoma. Case Rep Med. 2010;2010:121728.
- Tsukioka K, Takahashi K, Gomibuchi T, Kono T, Yajima T, Owa M. Mycotic Iliac Artery Aneurysm Caused by Clostridium difficile in a Patient with Axillobifemoral Bypass for Leriche Syndrome. Ann Vasc Dis. 2013;6(1):87-90.
doi pubmed - Lintin L, Wheeler R, Whiston R, Gordon A, Berry D, Torkington J. Mycotic thoracic aortic arch aneurysm from haematogenous spread of Clostridium septicum due to metastatic colorectal cancer: a survival guide. J Surg Case Rep. 2014;2014(11).
doi pubmed - Al Hadi HI, Patel G, Rees MD. A rare case of clostridium septicum mycotic aortic arch aneurysm following open right hemicolectomy for colorectal cancer. BMJ Case Rep. 2014;2014
- Subramaniam K, Hasmi AH, Mahmood MS. Clostridial aortitis causing ruptured dissecting aneurysm in a young adult female. Malays J Pathol. 2014;36(3):213-216.
pubmed - Shah S, Whitehead D, Sampath K, Toor A. A Case of Clostridium septicum Aortitis With Concomitant Adenocarcinoma of the Cecum. ACG Case Rep J. 2015;2(4):230-232.
doi pubmed
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Clinical Medicine Research is published by Elmer Press Inc.


